An Overview of Pulmonary Function Tests
General
Pulmonary function testing primarily detects two abnormal patterns:
- obstructive ventilatory defects (such as asthma and COPD) and
- restrictive ventilatory defects (such as
interstitial fibrosis and chest wall deformities).
Unlike some tests, pulmonary function testing is highly dependent on the
efforts of the patient and the technician performing the test.
Pulmonary function testing can be considered to be several tests in one.
What Is Normal?
The primary factors that determine what is normal for a given pulmonary function measurement are
Age,
Height and
Gender.
Weight is occasionally factored in, although wide variations in weight make little difference in the predicted normal value.
Various researchers have measured large groups of people to determine what is normal.
The sets of normal values most commonly used are:
- Knudson (1983)
- Crapo/Hsu
- Morris/Polgar
- NHANES III
I use Crapo/Hsu because it seems to be the most commonly used set in asbestos litigation.
Our local hospital uses NHANES III.
A study by
Frymyer from Presbyterian Hospital of Dallas found at
http://www.allegiance.net/respiratory/ab2002/OF%202002%20Group%2013/OF-02-117.html notes
"For spirometry, Knudson was used by 72% of the hospitals, Crapo 17%, Morris, Collins, ITS and Enright (CHS) were used by 6% of the hospitals. For DLCO, Knudson was used by 44% of the hospitals, Crapo 28%, Miller 11%, Morris, Collins, Burrows, and Polgar were used by 6% of the hospitals."
In general, if a given pulmonary function measurement is within 80% and 120% of the predicted value,
it is considered to be in the normal range.
This is a huge "point spread," but it is the best we can do.
For example, if an individual performs at 120% at age 20 and 80% at age 30, he or she is considered "normal" in both cases, yet has experienced a significant decrease in pulmonary function.
Spirometry/Flow Volume Loop
The patient takes a full breath in and blows out as long, hard and completely as possible.
He or she then takes a full breath in before resuming normal breathing.
This maneuver is done at least three times to be sure the results are
acceptable and reproducible.
Several numbers are generated including the FEV1 (the amount of air
exhaled in one second) and the FVC (the total amount of air one can take
into his or her lungs).
The entire maneuver is usually repeated after a medication called a
bronchodilator (albuterol) is given to open the breathing passages.
I tend to use the term "Spirometry" and the Sensormedics literature tends to use the term "Flow Volume Loop" to describe this test.
In truth, they are different represenatations of the same information -
"spirometry" referring to the numbers produced and "flow volume loop" meaning a graph produced by those numbers.
Maximum Voluntary Ventilation
This is often included under the above category, but it is a separate test.
The patient breathes as much air as possible in and out for a given amount of time.
It is possibly the least useful of these tests, although it can detect nervous system disorders.
Lung Volumes
The air that the lungs can hold can be divided into smaller compartments called "volumes."
"Capacities" are combinations of two or more volumes.
Since you will encounter these terms, I will discuss the important ones.
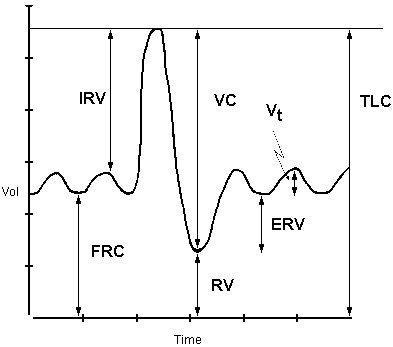
The amount of air a person breathes in and out during quiet, normal breathing is called the Tidal Volume (Vt).
Notice that during such breathing, a person could breathe more in or blow more out.
|
|
The additional amount a person could inhale is called the Inspiratory Reserve Volume (IRV).
The additional amount a person could exhale is called the Expiratory Reserve Volume (ERV).
After a person blows out all the air he or she can, there is still some air in the lungs.
This is called the Residual Volume (RV).
The Total Lung Capacity (TLC) is exactly what you would think - the total amount of air the lungs can contain.
The Vital Capacity (VC) is the total amount of air the person can breathe in and out.
The Functional Residual Capacity (FRC) is the total amount of air left in the lungs at the end of a normal exhalation.
If you prefer mathematical terms, get some help.
No, really here are the relationships:
- TLC = RV + ERV + Vt + IRV.
- VC = ERV + Vt + IRV.
- FRC = RV + ERV.
Diffusion Studies
Diffusion studies measure the ability of a gas to go from the air sacs of the lungs into the blood stream.
These studies do not really help differentiate an obstructive ventilatory defect from a restrictive ventilatory defect.
Instead, these studies give a clue as to what disease process within that category is present.
Pulse Oximetry
This is not usually considered a pulmonary function test.
It measures the amount of oxygen in small blood vessels called capillaries.
Since the lungs' job is to provide oxygen to the body, pulse oximetry is the ultimate test of pulmonary function!
Interpreting The Test
In general, this is my approach to interpreting a pulmonary function test:
First, I look at the FEV1/FVC ratio.
If this is below 75%, an obstructive ventilatory defect is present.
If the ratio is above 75%, are the FVC and FEV1 low?
If so, a restrictive ventilatory defect is likely and I next look at the lung volume section.
A low Vital Capacity confirms a restrictive ventilatory defect.
Some regard the Total Lung Capacity as confirmatory, so I consider both.
In general, in a restrictive ventilatory defect, the majority of lung volumes will be decreased.
If an obstructive ventilatory defect is present, the Residual Volume will be high.
I also look at the shape of the flow volume loop to differentiate an obstructive ventilatory defect from a restrictive ventilatory defect. An obstructive ventilatory defect gives a distinctive pattern. A restrictive ventilatory defect looks like a normal flow volume loop, except that it is smaller.
As far as diffusion studies, a low DLCO can be seen in both emphysema and interstitial fibrosis.
The DLCO can help differentiate the cause of a restrictive or obstructive ventilatory defect.
In a restrictive ventilatory defect, interstitial fibrosis may cause a decrease in DLCO but
chest wall deformities and obesity would not.
In an obstructive ventilatory defect, emphysema may cause a decrease in DLCO but
asthma would not.
The DLCO/VA is an attempt to correct the diffusion for the actual lung volume being tested.
A normal value should imply that the cause of the restriction is extrinsic to the lungs (such as a chest wall deformity or obesity) instead of intrinsic to the lungs (emphysema and interstitial fibrosis).
However, a normal value can occur in any of these conditions.
prada on sale prada heritage glasses prada collaborations prada vitello red fruit with hair prada svg brown prada shoes tamagotchies prada massage spa prada cleo crystal speqtrum prepress production services gorras prada mujer chatgpt prompts github prada purse cheap prada diris chatgpt cheat sheet prada leather mules gucci heuptasje rosemont lunch instagram million followers prada watch ladies chatgpt free online cost of chatgpt prada earmuffs million instagram followers prada 1999 captain hat dan prompt chatgpt prada authenticity prada crossbody wallet fiverr instagram followers bill gates chatgpt gucci com mosaic locations in florida prada bag 2005 bloomingdales prada sunglasses marca prada american native band featuring walela amazing grace in cherokee prada chess set pleasant hawaiian holidays aaa the gucci store prada espadrilles sale sailing captain hat prada camarillo outlet chatgpt sql gucci e commerce prada ambassador custom cork boards remove instagram followers in line commercial construction ferragamo shoes outlet prada supernova bag prada swirl sunglasses outlet belt cmyk reflex blue instagram ranking followers gucci com outlet prada san marcos non followers instagram prada infusion prada crystal sandals women gucci com firehouse subs fowler captain uniform prada sunglasses ladies nike outlet shoes online gucci offiziell tienda prada prada wallet sale prada red loafers valentino woodbury commons cinnabon mix cork board roll aeropostale factory million instagram followers at printing prada triangle perfume chatgpt excel plugin prada paradoxe notes tamagotchi pet instagram followers plus online clothing outlet stores prada jordans fuzzy prada bag rambutan ripe sheet of cork board prada socks mens prada tennis williams chicken dolce and gabbana spring summer 2015 fila prada instagram get followers growing colors by bruce mcmillan instagram automatic followers gucci things yellow prada purse prada men's sunglasses ship captain uniform prada slippers women tackboard
Examples
These are actual pulmonary function tests performed in my office.
The patient's identity has been protected by changing, at the minimum, the name and the date.
The HIPPAA folks would be pleased...
This page was created as aid to my employees when we started doing pulmonary
function testing in July of 1998. If this is helpful, feel free to use it.



